It became extremely important to learn “what is severe hypoglycemia”, how to recognize it, and ultimately how to treat it when our young grandson was diagnosed with Type 1 Diabetes.
 We discovered that by frequent monitoring of blood glucose levels, “lows” can be treated before they become severe.
We discovered that by frequent monitoring of blood glucose levels, “lows” can be treated before they become severe.
We also became painfully aware of just how quickly blood glucose levels can change.
I was quite surprised when I learned just how often Severe Hypoglycemia occurs. In fact, 58% of people with Type 1 and 29% of people with Type 2 diabetes have a severe Hypoglycemic episode.
Therefore, anyone who is taking insulin or insulin-releasing medication is at a heightened risk.
Even more scary is the fact that sometimes non-diabetic kids can experience Ketotic Hypoglycemia which simply means low blood sugars as a non-diabetic.
This makes it extremely important for us all to understand what is hypoglycemia and what can we do about it.
Table of Contents
What is Severe Hypoglycemia
Severe Hypoglycemia occurs when a diabetic has blood glucose(sugar) levels so low that they require assistance from another person in order to treat.
It is considered a medical emergency and is a complication of diabetics who take insulin or certain anti-diabetic tablets.
It is important to note that hypoglycemia can occur at any time but can often be a result of not eating meals on time, taking too much insulin for the amount of food eaten, or more exercise than planned for.
Hypoglycemia can even occur at night while the person is sleeping.
This is why our little grandson needs to have his blood glucose checked frequently throughout the night. Yes, he has had to be woken up to have some juice because he was too low. It can and does happen so be diligent with monitoring blood glucose.
Symptoms of Hypoglycemia
There are three levels of hypoglycemia.
- Level 1 (mild)
- blood glucose is less than 70 mg/dL but more than 54 mg/dL
- may experience sweating, shaking, nausea, extreme hunger, nervousness, dizziness
- Level 2 (moderate)
- blood glucose is less than 54 mg/dL
- may experience some of the above as well as difficulty concentrating or speaking, confusion, weakness, vision changes, mood swings
- Level 3 (severe)
- the person is unable to function because of mental or physical changes
- this is where the person is unable to take fast-acting sugar themselves and requires assistance, they may be unconscious or have seizures. They need to be treated with a Glucagon Emergency Kit.
It is important to realize that some people may experience some or all of these symptoms and some only a few.
Other people don’t feel anything out of the ordinary and this is called hypoglycemia unawareness, this is the case with our grandson. This could be due to his young age and he just doesn’t recognize the different feelings yet.
Testing blood glucose levels frequently is especially important in this case.
Is Hypoglycemia an Emergency?
Because untreated hypoglycemia can lead to seizures and death it is definitely a medical emergency.
Mild to moderate cases can be treated at home by taking fast-acting sugar or juice.
Severe cases of hypoglycemia require emergency treatment with a Glucagon Emergency Kit as well as hospitalization.
Treatment of Hypoglycemia
Severe hypoglycemia is a medical emergency. The main focus of the treatment is in raising the person’s blood glucose levels quickly with a medication called Glucagon. 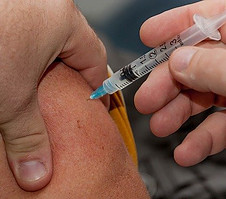
As a family member or friend or caregiver, you will have to step up and treat the person because they are unable to act on their own.
Call 911 or the local emergency immediately upon noticing the person unconscious. Glucagon kits are available by prescription and the Diabetic person likely has one nearby.
Glucagon is medicine usually given by injection, oral tablets, or nasal format. It is important to know how to use a Glucagon Emergency Kit so you are able to act quickly in an emergency to help raise the person’s Blood Glucose. They should regain consciousness within 5 to 15 minutes.
Once they are awake have them eat fruit, candy, or juice to help raise their sugars further. Be sure to test the blood glucose after 15 minutes to be sure it is rising.
How To Use a Glucagon Emergency Kit
When you first discover the person unconscious test their blood glucose levels to confirm that is the reason for their unconsciousness.
Then call 911 or local emergency in your area.
You are then ready to administer the Glucagon Emergency kit.
A glucagon Kit most often contains a vile of Powdered Glucagon and a syringe filled with saline (saltwater). Other kits may contain auto-injector or nasal spray, check the instructions for how to use these.
Steps to use an injection kit:
- Check the expiration date on the label to ensure it isn’t expired.
- Remove vial and syringe from the kit.
- Remove the covers from both the needle and the vial.
- Insert the needle into the vial and push the plunger to move all of the salines into the vial. Remove the syringe from the vial.
- Mix the saline and powder by gently rolling or swirling the vial until all of the powder is dissolved and the liquid looks clear.
- Insert the needle back into the vial and draw all of the liquid into the needle.
- Remove the syringe from the vial.
- Inject the needle into the outer portion of the person’s thigh, midway between the hip and the knee, or into the arm muscle.
- Place the person into the recovery position and watch for them to wake up. It may take from 5 to 15 minutes for the Glucagon to work and the person to wake up. Be sure to stay with the person until medical help arrives.
Once the person is awake it is important to get them to eat something like a piece of fruit, candy, or fruit juice to help further raise their blood glucose. Be sure to test their blood glucose after 15 minutes to ensure it is rising.
Conclusion
While Severe Hypoglycemia is serious, it can often be avoided by frequent monitoring of blood glucose. I know I kind of harp on blood glucose monitoring but yes it really is that important. By frequent testing, “lows” can be treated before they become emergencies.
Because of the seriousness of severe hypoglycemic episodes, it is imperative for family, friends, and caregivers to become familiar with symptoms and know exactly what to do for your Diabetic person should the need ever arise. By knowing what to do you will be able to act quickly and confidently and will ultimately save the person’s life.
I am not in any way a medical practitioner, please do not rely on the information on our website as an alternative to medical advice from your doctor or another healthcare provider. We only share our experiences.
Thanks for dropping by, you can leave your questions or comments below.


Hi Deborah,
Really good information on hypoglycemia here.
I did not know this could occur while you sleep and that some do not experience any symptoms!
Is it possible for non-diabetics to experience a hypoglycemic episode as well?
Thanks for the instructions on how to use a glucagon emergency kit — god forbid I ever have to use one, but now I feel confident in the process if the situation does occur.
Thanks for the info!
Anna
Thanks for the comment Anna.
While not common, it is possible for non-diabetics to experience Hypoglycemia.
There is Fasting Hyperglycemia that can occur 8 or more hours after eating.
There is also Reactive Hypoglycemia which typically occurs 2-4 hours after a meal and their body produces too much insulin.
This can be an indicator of developing Diabetes.
If you or someone you know has experienced the symptoms mentioned in the article get checked out by a doctor.
Thanks again. Deborah
Hello, thank you for this article. I did hear about severe hypoglycemia but to be honest I didn’t know much. You provide great peace of information. People need to know how to treat this condition, and that this is a medical emergency. Especially how to use Glucagon Emergency kit.
Best regards
Srdjan
Thanks for the comment Srdjan.
I am glad I could help clarify what hypoglycemia is and how to use a Glucagon Emergency Kit.
It is valuable information that could save a loved ones life.
Best wishes.