What is a diabetes management plan? Why do we need one? How do we manage our child’s diabetes when at school? Do type 1 and type 2 have different treatment plans? How do we treat highs? How do we treat lows?
These are just a few of the questions that may arise when someone is newly diagnosed with diabetes.
I know within our own family we asked these and many more questions in the days and weeks following the initial diagnosis of our grandson.
Imagine you are a builder and you are trying to build a house without any blueprints. How successfully do you think you will be?
We all understand the blueprint is the key to designing and building an attractive house that is structurally sound. If you ignore following that blueprint you could end up with a potentially dangerous house.
Trying to manage diabetes without a diabetes management plan would be very much like that builder trying to build without a blueprint.
Oh, you may have a basic idea of what to do but without that plan, you may be doing things incorrectly or in the wrong order, at the wrong times.
We have learned that with diabetes it isn’t just knowing what to do but also you must know when to do it.
A diabetes care plan will give you that knowledge.
Each plan is not only specific to the type of diabetes but also specific to each patient. Everybody’s body responds differently to treatments so the plan needs to be specific to their needs.
Some people will check blood glucose only with finger pokes, some will use a CGM (continuous glucose monitor) and others will use a combination of both.
Treatment plans may also vary in insulin delivery systems or when insulin is taken, always work with your doctor.
Table of Contents
What is diabetes?
The first thing we need to understand is what exactly is diabetes?
To put it simply, diabetes is when the body either doesn’t produce enough or any insulin or is unable to use it efficiently.
This leads me to the different types of diabetes.
Type 1 diabetes is when the body’s immune system attacks and kills the insulin-producing cells within the pancreas.
Our bodies use glucose (sugar) from the food we eat for energy. We need insulin for that sugar to enter the cells, it acts as a gateway so to speak.
Without that insulin, the glucose can’t enter the cells and it accumulates to dangerous levels within the blood. This can increase the risk of many life-threatening complications.
With type 2 diabetes the body doesn’t respond to insulin as it should causing increased blood glucose levels again risking many complications.
Type 2 diabetes is often a result of poor lifestyle choices and obesity. For this reason, it can sometimes be reversed through a healthy diet and regular exercise.
In either case, they share many symptoms which include:
- increased urination
- excessive thirst
- increased hunger
- blurred vision
- fatigue
- numbness or tingling in hands or feet
- sores that don’t heal
- unexplained weight loss
It is important that if you or someone your love is having any of these symptoms, please see your doctor as soon as possible.
What is diabetes management?
Diabetes and the complications of unmanaged diabetes can affect almost the entire body.
This means that it is important to properly manage blood glucose (sugar) levels to reduce the risk of developing complications.
It is also important to manage your blood pressure and cholesterol levels as well.
You can read more information about the complications of diabetes here.
The biggest part of diabetes management is being aware of how your body responds to everything you do. You must always be aware of how the food you eat and the activities you do affect your blood glucose.
This is what makes a diabetes care plan so essential.
What should a diabetes care plan include?
Almost everything you do can affect your blood glucose levels. This means there are many parts to a diabetes care plan. Each area needs to be addressed to obtain optimal results in managing blood glucose.
Food
Naturally, eating a healthy, well-balanced diet is key to any healthy lifestyle but for diabetics, it is a critical part of diabetes management. It is not only the types of food you eat that matter but it is also important to pay attention to portion sizes and combinations of food choices.
You will need to learn about carbohydrate counting and portion sizes. This is important because carbohydrates have the biggest impact on your blood sugar levels. As a family, we had to master carb counting early on as Alex’s insulin dosage is based on his carbs eaten at each meal.
The carb counting is so much easier if you take the time to learn what is the appropriate portion size for each type of food.
Create well-balanced meals and include plenty of fruits and non-starchy vegetables, whole-grain bread and pasta, brown and wild rice, lean proteins, and healthy fats. Ensure you get plenty of fibre to help keep your blood sugar levels more stable.
You will learn to coordinate your food with your medications. Too little food in proportion to your medications could result in a serious hypo event.
Your diabetes team will help you determine the best meal and medication schedule for you.
Drink plenty of non-sweetened beverages such as water, unsweetened coffee, or tea. The exception to this would be treating a low. Whenever our grandson’s sugars go too low a few sips of apple juice is all he needs to start raising those levels to within range again.
Exercise
This is another important part of diabetes management. This is because your muscles use glucose(sugar) for energy. Regular exercise can also help you use insulin more efficiently. Even light activities such as housework or gardening can help lower blood glucose levels so pay attention.
It is important to talk to your doctor about what type of exercise would be most appropriate for you. Typically, adults should aim for 150 minutes per week of moderate aerobic exercise. That works out to about 30 minutes a day for weekdays.
Follow your doctor’s recommendations for the right balance of aerobic and muscle building exercise for you as well as the best time of day for you to exercise.
Know your numbers before you start exercising because exercise can typically cause blood sugars to drop. Be sure you aren’t too low before beginning.
Whenever your exercise is sure to check your blood glucose before, during, and after any form of exercise. Pay attention to how your body responds to various types of exercise.
Drink plenty of water while exercising to avoid dehydration.
Always have a fast-acting sugar snack available to treat a low should it occur.
Your doctor will advise you on whether any alteration to your medications is necessary due to exercise.
Always work with your diabetes care team and follow their recommendations.
Medication
Properly managing diabetes often requires insulin and possibly other medications to be taken on time and in the proper dose.
Diabetes medications are also temperature sensitive so it is important they do not get too overheated or too cold(frozen).
Never leave your medications in the car.
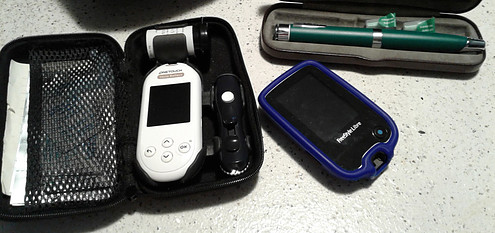
We use an insulated bag to take diabetes supplies everywhere we go. This ensures they don’t overheat in summer or freeze in winter.
Always check with your doctor before taking any over-the-counter medications.
Illness
When we are sick, our bodies produce stress hormones that can raise our blood sugar levels. Sometimes illness causes us to lose our appetite which can complicate diabetes management.
it is important to work with your healthcare team to determine your sick day plan.
This would include what medications you can take, how often to check blood glucose levels, when to check ketone levels, how to adjust your medication doses, and when to call your doctor.
It is important to continue taking your medications as usual and be sure to contact your doctor if you are experiencing nausea or vomiting.
It is important to follow your diabetes meal plan as much as possible. Stock up on food s that are easy on your stomachs such as gelatin, soups, crackers, and applesauce.
Drink plenty of water and other unsweetened beverages.
If you are taking insulin you may need to sip fruit juice to avoid going too low.
Alcohol
Normally, the liver releases stored sugar to compensate for falling blood sugar levels. However, if the liver is occupied trying to metabolize alcohol your blood sugar may not get the boost it needs which can result in a low shortly after drinking and for as long as 24 hours afterward.
Be sure to get your doctors okay before indulging in alcoholic beverages
Never drink on an empty stomach. Be sure to have a meal before or with that drink.
Check blood glucose levels before, during, and for up to 24 hours after consuming alcoholic beverages.
Carefully choose your drinks. Light beer and wine have the fewest calories and carbohydrates than other mixed drinks. If you really must drink spirits then try mixing with diet soda, diet tonic, club soda, or seltzer as these mixes won’t raise your blood sugars.
Keep a tally of your calories and carbs from drinks in your daily calorie count.
Be sure to check your blood sugar before bed. If it isn’t between 5.6 and 7.8 mmol/L have a snack before bed to counter a drop in blood sugar levels.
Menstruation and Menopause
During the week before and the week after menstruation and during before and during menopause hormone levels fluctuate significantly which can affect blood sugar levels.
Keep track of your blood sugar levels from month to month. This will help you predict what your sugars may do month to month.
Your doctor may recommend changes to your meal plan, activity level, or medications during menstruation.
Because the hormonal changes can drastically affect blood glucose levels it is wise to check your numbers more frequently.
Symptoms of menopause can often be confused with low blood sugar. For this reason, always confirm a suspected low before treating it.
Some oral contraceptives can cause higher blood sugars in some women.
Work with your doctor for the appropriate way to deal with these issues for you.
Who is the diabetes care team?
A diabetes care team is essentially a list of doctors and professionals who support you on this journey.
Your team could include:
- your family doctor
- a pediatrician
- an endocrinologist
- a nurse practitioner
- a certified diabetes educator
- a dietitian
- your local pharmacist
Any or all of these health care professionals will make up your diabetes care team.
It is important to work closely with them and follow all recommendations.
If you discover some aspect of your treatment plan isn’t quite working for you it is important to discuss this with your team. Never make adjustments to your plan on your own, ALWAYS consult your team.
Diabetes and school
Diabetes Canada recommends that each diabetic student has a completed diabetes care plan at school.
The child’s parents would get that plan filled out by their child’s doctor.
Once that is completed the parents should also fill out this quick reference sheet which outlines the common daily tasks for that child’s diabetes management while at school. A copy of this should be kept in the classroom and all places the child will be spending time throughout the day(library, gym).
It is also important to check whether your province has any additional specific requirements for documentation.
Final thoughts
I believe we have addressed the question “What is a diabetes management plan”?
Your diabetes management team will be comprised of several health care professionals including your family doctor, endocrinologist, diabetes educator, dietitian, and others.
Together they will formulate an individual plan that is unique to you and your needs.
This very individualized plan will help you manage your diabetes daily.
Your diabetes care plan will include diet, exercise, medication, illness, alcohol, and school/work.
This plan is what you will do daily to manage your diabetes and lessen the risk of developing complications.
I am not in any way a medical practitioner, please do not rely on the information on our website as an alternative to medical advice from your doctor or another healthcare provider. We only share our experiences.
Do you follow your diabetes care plan?
Do you follow the advice of your diabetes care team?
Do you have any tips or suggestions to help make daily diabetes management easier?
Leave your tips or suggestions in the comment section below.


Hi Deborah,
It occurs to me that many of the aspects of the diabetes management plan is typically how the majority of people (whether they are diabetic or not) should look to live their lives.
I’m referring to factors such as eating a healthy, well-balanced diet, ensuring we get plenty of exercise, and being aware of our alcohol consumption.
In fact, and please correct me if I’m wrong, I believe that not adhering to many of these principles could actually be the trigger for pre-diabetes or diabetes itself.
I come from a family that has a history of diabetes, but “touch wood” it hasn’t travelled down the family tree to my generation and beyond (yet).
However, I was wary of my late-mother and late-uncle not following a healthy, nutritious diet, or getting much exercise for that matter.
They suffered with Type 2 and Type 1 respectively.
Unfortunately, even once diagnosed, they didn’t follow a sensible diabetes management plan, so I know only too well how important this is.
It’s interesting that you also talk of the diabetes care team and how it’s important to work closely with them, but yet again this isn’t something that members of my family did very well.
Although, I would hazard a guess that there have been vast improvements in medical care over the past two decades.
A really interesting and informative read Deborah, and something that really resonates with me.
Thank you
Partha
So grateful you stopped by Partha and took the time to comment.
I agree that eating a healthy well-balanced diet, ensuring we get regular exercise, and controlling our alcohol consumption are habits everyone should adopt whether or not they are diabetic.
You are correct in stating that type 2 diabetes can often be avoided and even sometimes reversed by making these healthy lifestyle choices. I am sorry to hear that you had to witness family members neglecting to take care of themselves and their diabetes.
My mother did not take her type 2 diabetes seriously either and it was heartbreaking.
My father did not educate himself on how to properly manage her diabetes and often times he would mistake low blood sugars for cognitive decline due to Alzheimer’s Disease. It frustrated me when he would comment that she was fading when one glance told me she needed sugar immediately.
I would give her orange juice and she would almost immediately be back to her usual cheerful self.
I am grateful my daughter has taken our grandson’s type 1 diabetes seriously since the day he was diagnosed. While we have always eaten relatively healthy it has become more so since Alex’s diagnosis.
I wish you and your family continued good health.
Hi Deborah, this is a very thorough article on every aspect of diabetic care, my mother was a diabetic, I can’t remember her taking any medication for her diabetes,
I am also am diabetic, I remember when my dr told me I was pre-diabetic and gave me instruction on what I needed to do I didn’t follow his instruction either, and now I realize I acted foolishly
Great article,
Thanks for dropping by Ruthlyn.
I am sorry to hear your mother was a diabetic. You said you don’t recall her taking any meds. It sounds like she may have had Type 2 Diabetes which can sometimes be managed with diet and exercise alone and only require meds when it is more severe.
Thank you for sharing your own experience with what can happen when a pre-diabetic ignores doctors’ instructions. However, now that you are diabetic, it is imperative to follow your treatment plan exactly as your doctor has stated.
Learning to live with diabetes can be tricky at first but it doesn’t take long before it is second nature.
Oh, you will always have to watch what you eat and drink, get regular exercise, and limit alcohol consumption but those are part of any healthy lifestyle and shouldn’t be considered solely for the diabetics.
With proper management, it is possible for diabetics to avoid many of the complications and lead healthy lives.
Remember, you may have diabetes but it is up to you whether diabetes has you.
Best wishes.