I set out to learn the history of diabetes treatment and was absolutely shocked when I discovered the life-saving treatment my grandson receives is less than a hundred years old.
It is important to realize that until 1922, insulin had not yet been discovered so if you were diagnosed with diabetes, it was pretty much a death sentence.
And within a fairly short time period, we’re talking weeks or months here.
There was no treatment available.
On June 20, 2019, our daughter was devastated as she learned her 4-year-old son had type 1 diabetes.
Let me tell you, that diagnosis is scary enough nowadays, I can’t even imagine the devastation a parent would have felt a hundred years ago at hearing that diagnosis.
It was a death sentence, which meant that likely within a week you would no longer have that child with you.
Thank God for the work of Frederick Banting, John James Rickard Macleod, and Charles Best which led to the discovery of insulin.
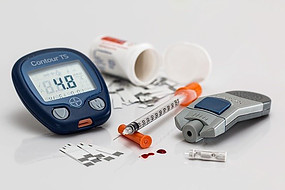
Today’s diabetics are fortunate to have treatment available and much easier methods of testing and controlling their blood glucose levels.
Let’s go ahead and check out this fascinating history.
Table of Contents
Origin of Diabetes
In the first century A.D., ancient Greek physician Aretaeus vividly described the destructive nature of an illness which he named “diabetes,” derived from the Greek word “siphon” (meaning flowing through), and rendered the earliest account of diabetic patients’ intense thirst and “melting down of flesh and limbs into urine.
Essentially a diagnosis of diabetes was a death sentence. Early attempts at treating it were futile and patients rarely lived beyond a few weeks or months after diagnosis.
In the middle ages, diabetes was known as the “pissing evil” and until the 11th-century diabetes was diagnosed by “water testers”, whose job it was to taste the urine of suspected patients to determine if it was sweet like honey.
Thus, the Latin word “Mellitus”, which means honey, was added to the word diabetes.
We now know Type 1 diabetes as Diabetes Melitus.
In “The Canon of Medicine” Avicenna provided a very detailed description of diabetes mellitus including abnormal appetite, the decline of sexual functions, and sweet urine. Diabetic gangrene was also identified.
Avicenna was the first to accurately describe diabetes insipidus.
It wasn’t until much later in the 18th and 19th centuries that Johann Peter Frank was able to accurately differentiate between diabetes mellitus and diabetes insipidus.
Today we call them Type 1 diabetes and Type 2 diabetes.
Symptoms of Diabetes
There are two main types of diabetes and while they have two different causes they have similar symptoms.
Type 1 diabetes
Type 1 diabetes occurs when the body’s immune system attacks and kills the insulin-producing cells within the pancreas. Insulin is required for the body’s cells to receive the glucose(sugar) from the food we eat to be used as energy. Without insulin, the glucose remains in the blood raising the levels significantly and causing many complications.
Type 2 diabetes
Type 2 diabetes is often caused by unhealthy lifestyle choices such as an unhealthy diet and lack of exercise which leads to being overweight. In type 2 diabetes, the body either doesn’t make enough insulin or it can’t effectively use that insulin causing blood glucose levels to rise.
In either case, blood glucose rises and several life-threatening complications can arise.
The symptoms of diabetes are:
- increased urination
- excessive thirst
- increased hunger
- blurred vision
- fatigue
- numbness or tingling in hands or feet
- sores that don’t heal
- unexplained weight loss
If you or someone you love is having any of these symptoms, please see your doctor as soon as possible.
While there is still no cure, diabetes can be managed and many of the complications avoided.
I recall our daughter telling about our grandson suddenly needing to often pee, like every 10 or 15 minutes.
He was also extremely thirsty. He would gulp down glasses of water like he had been stranded on a dessert, yet he had a glass of water 5 minutes ago.
Our daughter recognized these symptoms and immediately made a doctors’ appointment.
The doctor did a finger poke to check blood glucose levels and they were through the roof at 28 mmol/L, normal would be between 5-7.
He was sent straight to the hospital for further testing and was diagnosed that same day with type 1 diabetes.
Early Diagnosis
The first documented mention of the symptoms of diabetes was by Egyptian physician, Hesy-Ra in 1552 B.C. He reported frequent urination and extreme weight loss as a symptom of a mysterious disease.
Also, ancient healers of about the same time period noticed that ants were attracted to the urine of people with this same disease.
Step forward in time to 150 A.D. when Arateus, a Greek physician described what we now call diabetes as “the melting of flesh and limbs into urine”. It is from this point that doctors began to understand diabetes a little better.
Centuries later, diabetes was diagnosed by “water tasters”, people who literally tasted the urine to see if it was sweet.
In 1675, the word “Mellitus” was added to the word diabetes creating the modern name of Diabetes Mellitus.
Scientists developed chemical tests for diagnosing diabetes in the 1800s.
Early Treatments
It took a very long time for diabetes treatments to develop to where they are today.
The very first diabetes treatment was prescribed exercise, often horseback riding, which was thought at the time to relieve excessive urination.
Finally, by the 1700s and 1800s, doctors’ started to realize that dietary changes could help manage diabetes.
Doctors would prescribe that their patients eat only the fat and meat of animals or consume large amounts of sugar.
During the Franco-Prussian War of the 1870s, Apollinaire Bouchardat, a French physician, noted his diabetic patients’ symptoms improved with the war-related food rationing. He then developed individualized diets as diabetic treatments.
Naturally, this led to several fad diets in the early 1900s such as “oat-cure”, “potato therapy” and the “starvation diet”.
In 1916 a Boston scientist named Elliott Joslin created a textbook entitled The Treatment of Diabetes Mellitus. This book states that a fasting diet combined with regular exercise can significantly reduce the risk of death in diabetes patients. These principles are still used today when teaching patients about necessary lifestyle changes for managing diabetes.
As you can well imagine, before the discovery of insulin, people with diabetes often died within a few weeks or months of diagnosis.
Discovery of the pancreas’ role
In 1889, Oskar Minkowski and Joseph von Mering, researchers at the University of Strasbourg in France, discovered that removing the pancreas from a dog could induce diabetes. This was the first big breakthrough leading to the discovery of insulin because we now know where to look for a solution as this pancreas seems to be the cause.
In the early 1900s a German scientist, Georg Zuelzer found that injecting the pancreatic extract into patients could help control their diabetes.
In 1910, it was discovered by Sir Edward Albert Sharpey-Schafer, that diabetes resulted from a lack of insulin. He named the chemical responsible for regulating blood sugar insulin after the Latin word “insula” which means island, referring to the insulin-producing Islets of Langerhans in the pancreas.
A physician from Ontario Canada, Frederick Banting came up with the idea to use insulin to treat diabetes in 1920. He and his colleagues began animal experiments testing his theory.
In 1922 Banting and his team successfully treated a diabetic patient and the following year they were awarded the Nobel Prize in Medicine.
Today we use a combination of daily insulin injections, diet, and exercise to treat type 1 diabetes, while type 2 diabetes is often treated with diet and exercise alone.
Today’s treatments
Today regardless of which type of diabetes you have you will need to frequently check your blood sugar levels. This is where the similarities end though, the treatment of each type is different.
Your diabetes care team will develop a diabetes treatment plan specifically designed for your case. This is because each case is unique and everyone’s body responds differently to a treatment.
Type 1 diabetes:
Your diabetes care team will tell you how often they want you to check your blood glucose levels. For our grandson, it is quite frequently:
- when he wakes
- before each meal
- several times between meals
Before each meal, you will need to count the number of carbs you intend to eat so you can calculate your insulin dosage. Your doctor will give you your ratios that he wants you to use in calculating your insulin dose. Alex has a different ratio for each meal.
You will take your insulin dose either right before eating or as soon as you are finished. With Alex, we wait until he finishes eating so we know exactly how much he has eaten. As a 6-year-old he doesn’t always eat all of his meals. Waiting gives us the chance to weigh or measure uneaten carbs so we can make any necessary insulin adjustments. We don’t want to give him too much insulin.
You also take long-lasting insulin or base insulin shot at the time recommended by your doctor. With our grandson, it was early in the morning before he was even out of bed but it has since been changed to bedtime.
Eat a healthy, well-balanced diet.
Get regular exercise. Be sure to check your blood sugar levels before, during and after exercise.
Type 2 diabetes:
Your doctor will let you know how often he wants you to test your blood sugar levels. Be sure you do it.
Take all medications exactly as prescribed at the times prescribed.
Eat a healthy, well-balanced diet.
Get daily exercise.
Final Thoughts
As you can see from this article the history of diabetes treatment had a long and interesting journey.
While being diagnosed with diabetes was once a death sentence we have certainly come a long way.
All over the world, there is ongoing research into better treatments for diabetes and eventually a cure.
I am so grateful that we live in today’s world with modern medical technology to treat our grandson’s type 1 diabetes.
Alex follows a healthy diet, gets regular exercise, and has insulin injections several times a day.
He will continue to do this for the rest of his life unless they find a cure within his lifetime.
Our grandson is able to live a relatively normal life thanks to modern treatments.
When you look at him you can’t tell he has such a potentially life-threatening disease, he looks like any other kid.
I am not in any way a medical practitioner, please do not rely on the information on our website as an alternative to medical advice from your doctor or another healthcare provider. We only share our experiences.
While we have made huge advancements in diabetes treatment, I believe we’re on the cusp of developing a cure.
I am fascinated to see where further research takes us.
How do you manage your diabetes?
Diet and exercise?
Insulin injections?
A combination of all three?
Share your experience in the comment section below.

Hi Deborah,
I found this utterly fascinating.
I still recall my first real experience of seeing someone with diabetes, although I didn’t realize it at the time, and it wasn’t until many years later that I cottoned on to what was happening.
I couldn’t have been more than 5 or 6 and a young lad in my class typically always had to eat at different times from the rest of us (or so I thought), he always carried a lunchbox with biscuits in, and he often felt faint and was unable to take a full part in physical education classes.
Unfortunately, kids being kids, this poor boy was often ridiculed for being “different”.
I will say that this was the late 1970s/early 1980s, so treatment and knowledge have certainly come a long way since then.
I have also watched my late-mother and late-uncle develop and live with type-2 and type-1 respectively, and it was only during this period that I actually realised what a serious condition this was.
This led to me studying and researching diabetes in more detail, but more so for how to deal with people suffering from this affliction, and potential cures.
I must admit I knew absolutely nothing about the history of diabetes treatment, and you have certainly opened my eyes.
All I can say is that not only have we come a long way in the last century but let’s be thankful that there is no longer a requirement for “water testers”, LOL.
A thoroughly enjoyable and enlightening read Deborah, and my best wishes to your grandson.
Partha
Thanks for dropping by Partha. Yes, kids can be cruel when they don’t understand why someone may be different. I find today many people are teaching their kids to be more accepting of differences and so far in school our grandson hasn’t been teased by his peers. Unfortunately, this has not been the case with many adults as he is unable to ride the school bus useless my daughter chooses to place him on the ‘handicap” bus. Diabetes is not a handicap especially with today’s technology and treatment options. Still, there is a lot of misunderstanding which is the purpose of this site. I am very thankful we do not require “water testers” any longer. That would be a horrible job.
Hi Deborah,
Thanks for the reply.
I agree that the world is very different nowadays, and there’s definitely far more knowledge about diabetes.
With that said, there is still a great deal of ignorance and misunderstanding.
I think a prime example of this is how your grandson must travel to school.
Well, I think you’re doing a great job with the site, and I for one already feel more knowledgeable than before.
Thanks
Partha
Thanks again Partha for this wonderful conversation. I am extremely happy my site is helping to give you a more thorough understanding of diabetes. Knowledge is certainly the key to clearing up misunderstandings and eliminating ignorance. With enlightenment comes understanding and acceptance of differences. Thanks for dropping by again. Best wishes to you and yours.
Really interesting read, Deborah. Now that I have read several of your articles, slowly I am starting to understand what Diabetes is. I am lucky enough to not have a lot of experience with this disease.
It seems Diabetes 2 runs in my family. My niece told me the other day that her mother and an uncle had it and that she herself has it now as well. I am subscribed to a newsletter of a Dutch alternative doctor and he claims Diabetes 2 can be totally cured by the right lifestyle. You say in your article as well Diabetes 2 can be treated, but have you found evidence as well that this treatment leads to total healing?
Hi Hannie. I am so thankful you don’t have firsthand experience with diabetes. Sorry to hear your niece now has it and that you have other family members who had struggled with it in their lifetime.
In the case of type 2 diabetes, you are correct in that it can sometimes be reversed with healthy lifestyle changes. Whether or not it can be fully cured with lifestyle changes alone likely depends on the severity of symptoms and the length of time the person has had it.
I personally know several people who were able to reverse it and go off their diabetes meds.
Type 1 diabetes is a different game altogether. A type one diabetic does not produce enough or any insulin and so must take insulin injections several times a day. Healthy lifestyle choices will certainly make it easier to get those blood sugar levels within the target range but they never are able to go off insulin until such time as a cure is discovered.
Thanks again for dropping by.