Have you noticed how things are always changing in this fast-paced world we live in so I like to keep informed on what’s new in diabetes treatment?
It has been about a year and a half since our grandson was diagnosed with type 1 diabetes.
We have learned so much in that time, some things we learned from Alex’s doctors (via our daughter), and other things we learned by trial and error alongside our daughter.
As a family, we are feeling pretty comfortable in the day to day dealings of type 1 diabetes.
Diabetes really is all-consuming.
Alex endures 4 insulin injections, countless scans of his CGM and at least 4 finger pokes throughout an average day.
He can’t eat his meals until we have counted his carbs in order to accurately dose his insulin.
His snacks and meals must be on time or as close as possible.
If his scanner shows his going too low he is finger poked again and made to eat a snack whether he feels hungry or not.
If his sugars are too high we try getting him to drink more water, failing that he gets a small dose of insulin because we obviously didn’t give him enough at mealtime.
Yes, managing type 1 is very much like a guessing game. You try your best to calculate everything but it is diabetes and by nature, it can be unpredictable at best.
Oftentimes, what worked yesterday doesn’t work today so you try something else.
I wonder, what is new that may make living with diabetes easier in the future?
Table of Contents
Technology
We are all aware of how fast technology has been advancing.
Not just with computers and smartphones, but also within the medical field as well.
It was 20 to 25 years ago that my mother was diagnosed with type 2 diabetes. A lot has changed since then in treatment options available to both type 1 and type 2 diabetics.
There have been significant advances in medical technology throughout the last 10 years and we are fortunate that our grandson was diagnosed within those ten years.
So let’s take a look at options available now that perhaps were not available just 10 years ago.
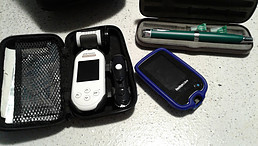
CGM’s(Continuous Glucose Monitors)
I believe these are a true game-changer.
So what is a Continuous Glucose Monitor(CGM)?
A CGM is a device that tracks blood glucose.
Alex wears a small disc that has a cannula (small sensor) just under the skin. The sensor sends the readings to a scanner (reader) that records the glucose levels.
This allows you to keep track of trends much easier than hand-graphing every finger poke result.
Some CGM’s, such as the Dexcom, can even send the info directly to your cell phone or even to your doctor.
Some can give alarms when blood sugars are heading too low, Alex’s does not which is why our daughter would prefer the Dexcom.
daughter would prefer the Dexcom.
Keep in mind, not all CGM’s are covered by every insurance carrier so check with your carrier before deciding which you would go with.
Our daughter really wanted the Dexcom but it isn’t covered on their insurance so they went with the Freestyle Libre system.
It kills me when I think of how often Alex needed his fingers poked when he was first diagnosed.
It absolutely broke my heart to see his little fingers looking like pincushions.
We were all so excited when his doctor suggested he start wearing a CGM and he is down to about 4 finger pokes a day, much easier on him and us.
It has been a welcome addition to Alex’s treatment plan and I would certainly recommend you discuss wearing A CGM with your doctor if you are not currently wearing one.
What is an Insulin Pump?
An insulin pump is a device that a diabetic can wear to deliver insulin automatically at preprogrammed times and doses or in response to commands given by the wearer or caregiver.
It has the capability of drip-feeding insulin throughout the day or gives larger doses at mealtimes.
Our grandson does not wear an insulin pump but he is starting to ask about one. My daughter is not yet convinced she wants a device to control her son’s insulin. They will likely discuss it at his next appointment.
More discreet pumps
The first insulin pumps were pretty clunky and cumbersome, at the time wearers called them “the blue brick”.
Today, insulin pumps have been redesigned with a sleek look, touch screen and smart tools:
- memory – allows you to save and even suggest insulin dosage for your favourite meal
- multiple basal settings for different background insulin profiles based on planned activities for the day
- communicates with a paired CGM (continuous glucose monitor)
Today there are many innovative creations to help make wearing a pump more comfortable and discreet and even fashionable:
- tubeless pumps
- belts
- clips
- specially designed pouches
 Nowadays, wearing a pump has become much less stigmatized.
Nowadays, wearing a pump has become much less stigmatized.
In 2014, Miss America semifinalist Sierra Sandison (Miss Idaho), walked the stage on national television during the swimsuit competition with her insulin pump proudly clipped onto her bikini bottoms.
Closed-loop systems
People can choose a pump that pairs with a CGM in order to build a system that not only constantly tracks blood sugars, but shares that data with the pump and then make decisions on behalf of the user, dosing insulin according to the data received.
An example would be the T-Slim Control IQ system that pairs with a Dexcom G6 device.
This type of system is called a closed-loop system or an artificial pancreas.
Living with diabetes requires a LOT of thinking and automatic insulin adjustments require considerably less thinking.
Many people report that overnight glucose levels are more stable when using a closed-loop system.
As more companies continue to develop new innovative products it is exciting to think of where diabetes management could go.
Be sure to ask your doctors about the latest technology available in your location.
Improved treatments
Just as there have been advancements in technology, there have also been advances in medical care.
Today`s treatments can be highly individualized as a result of better blood glucose data provided by the new technology.
Pen Needles
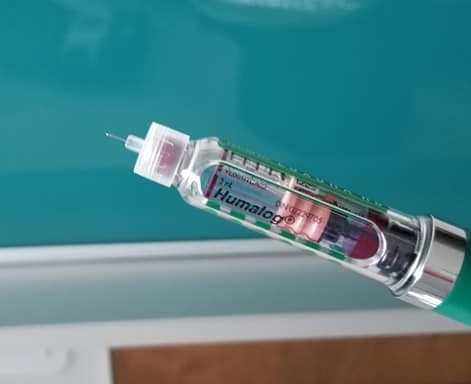 In my opinion, the insulin pen needle has been one of the most life-changing advancements in diabetic care.
In my opinion, the insulin pen needle has been one of the most life-changing advancements in diabetic care.
It was first introduced in 1985 by the Danish company Novo Nordisk.
More than 95% of the millions of diabetics worldwide are currently using pen needles.
This is likely because pen needles offer improved convenience and less pain than traditional insulin syringes.
Originally, pen needles were quite long and sharp but thanks to continued technological improvements they are now much smaller, thinner and often painless.
My favourite feature of pen needles is how convenient it is to change the actual needle with much less waste than traditional syringes and how convenient it is to just dial the dose and half doses are easily accomplished as well.
For us, this is important because Alex is only 6 and often requires a half dose. For example last night’s supper he required 3 1/2 units of insulin based on the carbs he ate.
Faster insulins
Did you know that before today`s rapid-acting insulins, diabetics would have to plan a meal, inject a half-hour before and wait before eating?
That is no longer the case.
Fast-acting insulins allow diabetics more flexibility not only in correcting high blood sugars but also in what they choose to eat. It also gives them the freedom to snack whenever they desire.
Today’s technology and medical advancements allow them to choose a snack, dial-up and inject insulin at that moment.
New treatment choices
There have been advances in medications prescribed to those with type 2 diabetes as well.
These new medications can help lower difficult-to-treat high blood sugar levels and may reduce the need for insulin for some individuals.
There is a new generation of diabetes medications that shows promise in treating people with other health issues (particularly those related to the heart and kidneys).
These new medications include:
- sodium-glucose cotransporter-2 (SGLT2) inhibitors
- glucagon-like peptide-1 (GLP-1) receptor agonists
These medications may also help prevent other complications of diabetes as well.
Hypoglycemia treatments

Until recently, severe hypoglycemia was treated by having to inject glucagon.
This was quite an ordeal because there were several steps involved that you needed to remember and perform in order while you are freaking out about your loved ones’ medical emergency.
Certainly not an ideal situation.
With Alex, we were each taught how to administer the emergency Glucagon Kit. Thankfully we never had to use it.
Today there is a couple of much easier options available.
There is a new Glucagon powder that can be administered through the nose that was approved by the FDA in 2019.
Also, there is a new injectable Glucagon also approved in 2019 by the FDA, that can be kept at room temperature and doesn`t require any mixing which is a huge improvement in my opinion.
Final Thoughts
I believe I have answered the question “what’s new in diabetes treatment”.
There have been tremendous advances in both technology and medical treatment available to diabetics.
CGM’s (Continuous Glucose Monitors) are a fantastic way to keep an eye on those blood sugar levels with considerably fewer finger pokes.
We have noticed a big difference since Alex has been wearing one. He feels more like a normal kid when you can just scan him rather than halting his play for a finger poke.
You should also consider an insulin pump.
There are pumps that can sync with a CGM and share data and make decisions on your behalf.
There have been new types of insulin and new medications available to type 2 diabetics as well.
Be sure you check with your insurance provider before deciding on anything because not all devices are covered by all insurance companies.
Work closely with your diabetes care team in order to find the right treatment plan for you.
Everybody responds differently to treatment which is why it is so essential that today’s treatment options be so individualized.
I am not in any way a medical practitioner, please do not rely on the information on our website as an alternative to medical advice from your doctor or another healthcare provider. We only share our experiences. If you purchase something from a link or ad on this site we may receive a small commission. This in no way affects the price you pay.
What experiences do you have with today’s technology?
Have you tried a CGM (continuous glucose monitor)?
Have you used an insulin pump?
Does it sync with your CGM?
Share your experiences in the comment section below and do take care of yourself.

The technology has really advanced in 10 years! Having a family history of diabetes, I remember many years ago, my aunt having to prick her finger all the time. As the years gone by and new medication and tech came out it has became so much more managable and not as dire as it was.
I am glad to pass by your page as my mother does have diabetes and now I want to talk to her about these other options!
Thank yoiu!
Thank you for dropping by and taking the time to comment. I am sorry to hear your Mom is battling the diabetes journey. I am sure her doctors will help her decide on the best treatment options for her. Everybody reacts differently to treatments so it really is very individualized now which is great. We are fortunate to live in times when technology can make treatments so much easier than in the past. I wish you and your family all the best. Take care.
Great article on whats new in diabetes treatment. I have a friend with diabetes so I’m going to recommend the CGM treatment. That seems like a great option to manage diabetes. Thanks for sharing this helpful info.
Have you done any articles on eating to manage diabetes?
Best wishes!
Thanks for dropping by Alyse. I am sure your friend will appreciate you recommending she ask her doctor about using a CGM (continuous glucose monitor).
As a family, we love it. We have noticed a huge difference, fewer finger pokes mean fewer tears from adults as well as Alex. Another bonus is we seem to catch potential hypo events before they get serious and this has made a positive impact on his A1C numbers.
In answer to your question, “Have you done any articles on eating to manage diabetes?”, yes I have written some articles on nutrition as well as various diets. Check out “Type 1 Diabetes Meal Plan“, “the Keto diet and diabetics” or “the Mediterranean Diet and Diabetics“.
I hope this helps. Take care.
Hi Deborah,
It’s great that I have came across this article as my cousin is diabetic, and I am not sure she knows about this treatment yet. She injects her medicine the traditional ways, but this could be a more effective and easier method.
I am going to share this article with my cousin and I will encourage her to comment on your post. If she likes it and starts to follow these new methods then I will let you know. If she has any questions then I will encourage her to get in touch with you. IF that is OK with you?
Thank you for sharing and keep up the great work.
All the best,
Tom
Thanks for stopping by Tom.
You mentioned your cousin is injecting her medication in the traditional way. One vast improvement that I forgot to mention and I will now go back and edit is the use of pen needles rather than traditional syringes. That is what we use for Alex. They are so easy to dial the dose rather than trying to accurately fill a syringe, eliminate any air and then inject intramuscularly. Thanks for reminding me.
Whether she opts for pen needles or an insulin pump I am sure she will find it much easier to manage her diabetes.
I am honoured that you would encourage her to get in touch with me if she has any questions. She is more than welcome to reach out any time.
Thanks again Tom and do take care.